Lactose-Free vs Dairy-Free: How to Find the Difference
We all often get asked about allergies, especially when dining at restaurants, coffee shops, and other establishments. As someone who is lactose and gluten-intolerant, I’ve noticed a common misconception in both the lactose-free and gluten-free communities: the confusion between lactose intolerance and a dairy allergy.
Many people use these terms interchangeably, but they refer to two distinct medical and nutritional conditions. Understanding the differences is crucial for health, safety, and effective diet planning.
This matters not only for people managing digestive symptoms, but also for anyone cooking for others, reading food labels. Misunderstanding the difference can lead to unnecessary food avoidance, nutrient deficiencies, or, in the case of dairy allergy, serious medical risk.
This article explains lactose intolerance vs dairy allergy in a clear, narrative way for the general public, while also reflecting evidence-based nutrition science and real-world dietary guidance suitable for a health-conscious, gluten-free, lactose-free blog.

Why Lactose Intolerance vs Dairy Allergy Is So Often Confused
From a nutrition education perspective, the confusion is understandable. Both conditions involve reactions after consuming dairy foods such as milk, cheese, or yogurt. Both may cause digestive symptoms. And both often lead people to say, “I can’t have dairy.”
However, the similarity ends there.
Lactose intolerance is a digestive issue related to how the body breaks down lactose, a sugar naturally present in milk and dairy products. Dairy allergy is an immune system reaction to milk proteins. One causes discomfort; the other can be dangerous. Understanding this difference is essential for making informed food choices and for protecting people with true allergies.
Many people with lactose intolerance can still tolerate certain dairy products, especially those that are fermented or naturally low in lactose. Foods like long-fermented yogurt, hard cheeses such as Parmesan, and clarified butter like ghee are often easier to digest when prepared properly.
Lactose Intolerance World Map
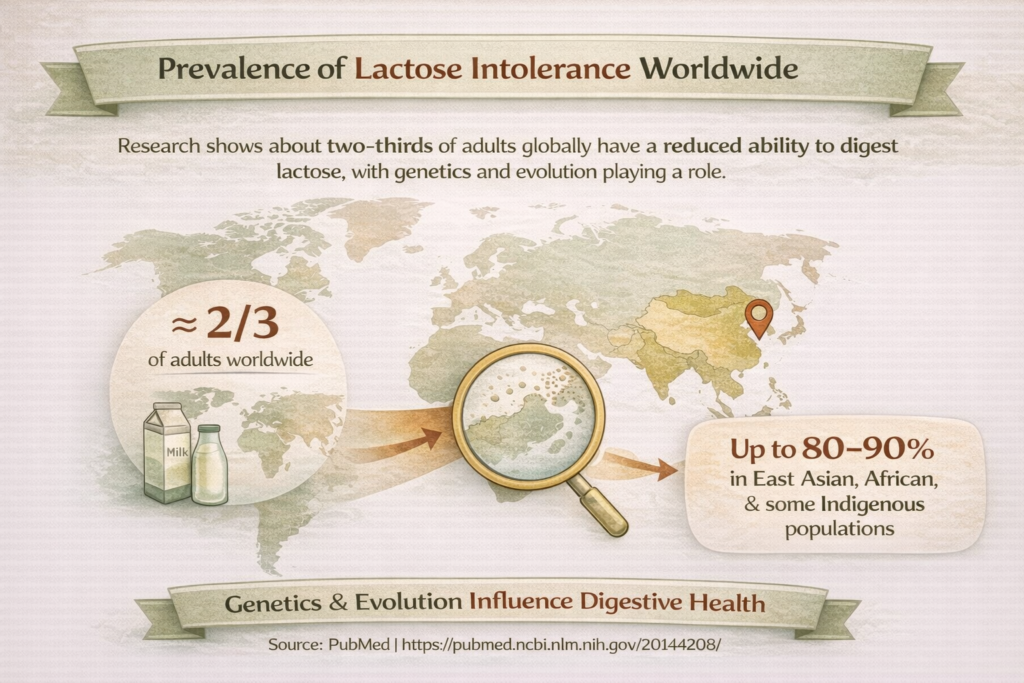
From a global nutrition perspective, lactose intolerance is incredibly common and often under-recognised. Research indicates that roughly two-thirds of adults worldwide experience some degree of reduced lactose digestion due to declining lactase enzyme levels after childhood. This doesn’t mean everyone will have symptoms, but the biological tendency is widespread.
Prevalence varies markedly between populations: it’s relatively low in Northern European groups, yet much higher (80–90%) in East Asian, African, and some Indigenous populations. Thus, highlight the influence of genetics and evolutionary adaptation on digestive health. Understanding this prevalence helps explain why lactose intolerance is such a frequently discussed concern in both clinical nutrition and everyday food choices.
Most people’s bodies gradually produce less lactase, the enzyme that digests milk sugar, as they age. This reduction in lactase production can make it more challenging to digest milk in adulthood.
However, certain populations have developed the ability to continue digesting milk because dairy has been a consistent part of their traditional diet for many generations. As a result, their bodies have genetically adapted to produce lactase into adulthood. This adaptation allows them to break down milk sugar more easily, so consuming milk does not cause the digestive problems that many other adults experience.
What Is Lactose Intolerance? A Digestive Health Perspective
Lactose intolerance occurs when the body does not produce enough lactase, the enzyme needed to digest lactose. Lactose is the natural sugar found in milk and dairy products.
Under normal conditions, lactase breaks lactose into two smaller sugars that can be absorbed in the small intestine. When lactase levels are low, lactose remains undigested and passes into the large intestine. There, gut bacteria ferment it, producing gas and drawing water into the bowel.
According to the National Institute of Diabetes and Digestive and Kidney Diseases, lactose intolerance is extremely common worldwide, particularly in adults. In fact, reduced lactase production after childhood is a normal biological process in many populations.
From a nutrition standpoint, lactose intolerance is not a disease or an immune reaction. It is a variation in digestion, and symptom severity often depends on the amount of lactose consumed.
A1 Casein Sensitivity
Some people who experience digestive discomfort after consuming milk do not fit neatly into the categories of lactose intolerance or milk allergy. In these cases, symptoms may be linked to sensitivity to A1 beta-casein, a type of milk protein found in most conventional cow’s milk. During digestion, A1 casein can release bioactive peptides that may irritate the gut lining and contribute to low-grade inflammation in susceptible individuals.
This reaction is not caused by enzyme deficiency and does not respond to lactase supplements. While research suggests that A1 is well tolerated by many people, those with sensitive digestive systems may benefit from choosing A2, goat, sheep, or fermented dairy products. This topic will be explored in more detail in the article “Casein, Inflammation, and Dairy Sensitivity: What the Science Really Says.“
Beyond Lactose: Dairy Proteins and the Gut Microbiome
Emerging research suggests that components of dairy beyond lactose, including small protein fragments called casomorphins, may interact with the gut and its microbial environment, influencing digestion and systemic health.
Casomorphins are released from dairy proteins during digestion and have been shown to bind opioid receptors throughout the gut and the rest of the body, potentially affecting gut motility, inflammatory signals, and microbial interactions within the intestine.
While this area of research is still evolving, it highlights that different constituents of dairy can have complex effects that extend beyond lactose alone and that the gut microbiome plays a key role in moderating how these food-derived peptides are processed and experienced by the body.
Common Lactose Intolerance Symptoms Explained
People with lactose intolerance typically experience symptoms within 30 minutes to two hours after consuming dairy. These symptoms are mostly limited to the digestive system and may include bloating, abdominal cramps, excessive gas, loose stools, and sometimes nausea.
Because gut bacteria play a central role in fermentation, differences in the microbiome can influence whether lactose causes mild discomfort or more pronounced IBS-like symptoms. I discuss this relationship in more detail in my article on the microbiome and digestive health.
While these symptoms can significantly affect quality of life, they are not dangerous. Importantly, many people with lactose intolerance can still tolerate small portions of dairy or certain dairy products without symptoms.
This is why blanket dairy elimination is not always nutritionally necessary for lactose intolerance.
Nutritional Value of Milk and Dairy
For people with lactose intolerance, avoiding all dairy products is not always necessary or beneficial for nutrition. Many low-lactose or lactose-free dairy products, such as long-fermented yogurt, hard cheeses, and lactose-free milk, still contain casein, the main protein in milk.
Casein naturally carries important minerals, including calcium, phosphorus, and magnesium, with most of milk’s calcium bound within casein structures.
These nutrients play a key role in bone health, muscle function, and metabolic processes. When tolerated, incorporating low-lactose or lactose-free dairy allows individuals with lactose intolerance to obtain these valuable nutrients efficiently, supporting a balanced diet without unnecessary restriction.
In the absence of a true dairy allergy, these forms of dairy can be an excellent, nutrient-dense addition to an intolerance-friendly eating pattern.
When and Why Dairy May Trigger Inflammation
Dairy is not inherently inflammatory for everyone, but it can contribute to inflammation in specific situations. For individuals with a dairy allergy, immune reactions to milk proteins can trigger inflammation throughout the body and must be avoided entirely.
In people with lactose intolerance, undigested lactose can cause gut irritation and local inflammation through bacterial fermentation, especially when large amounts of high-lactose foods are consumed.
Additionally, some individuals may experience inflammatory-type symptoms when consuming certain dairy products due to milk protein sensitivity, gut permeability issues, or underlying digestive conditions, even in the absence of a diagnosed allergy.
Importantly, for people who tolerate dairy well, especially fermented or low-lactose forms, dairy foods are not considered inflammatory and can be part of a healthy, nutrient-dense diet.
Considering how widespread lactose intolerance is worldwide, and how frequently dairy appears as an ingredient in everyday foods, it’s easy for some people to experience ongoing IBS-like symptoms without realising lactose is the trigger.
In many cases, digestive discomfort such as bloating, gas, or irregular bowel habits may be attributed to stress or “sensitive digestion,” when in fact undiagnosed lactose intolerance is the underlying cause — something I personally experienced myself, if you read my story.
Also, lactose intolerance is often confused with other food-related triggers, including gluten sensitivity. I explore this overlap in more detail in my article on gluten-related digestive symptoms and intolerance, where I break down how similar signs can stem from very different causes.
My Experience and Practical Food Guide for Lactose Intolerance
Because lactose intolerance affects sugar digestion rather than dairy proteins, many people tolerate fermented or low-lactose dairy well. These foods retain valuable nutrients while being gentler on digestion.
🚨These options are suitable only for lactose intolerance and are not safe for individuals with a dairy allergy.
The good news is that you don’t have to cut dairy completely. On my blog, you’ll find 24-hour fermented yogurt, and a lot of yogurt-based recipes.
Also, you might noticed that I have plenty of lactose-free cheese recipes, Parmesan gluten-free dishes, and ghee butter recipes designed specifically for sensitive digestion.
Do You love Cheese?
When casein is digested, it can release small peptides called casomorphins, which have mild opioid-like activity in the body. These naturally occurring compounds may influence gut movement and feelings of satiety or comfort after eating dairy. Sensitivity varies between individuals, and for people without dairy allergy, casomorphins are considered a normal part of milk protein digestion.
Emerging research suggests that casomorphins, may interact with the gut and its microbial environment in ways that influence digestion and systemic health.
While this area of research is still evolving, it highlights that different constituents of dairy can have complex effects that extend beyond lactose alone and that the gut microbiome plays a key role in moderating how these food-derived peptides are processed and experienced by the body
Lactose Intolerance Offenders
Most Likely Highest lactose content, the fastest symptom trigger
- Regular milk (especially skim and low-fat milk)
Milk contains a high amount of lactose, and lower-fat versions empty from the stomach faster, which can worsen symptoms. - Evaporated milk and condensed milk
These are highly concentrated sources of lactose and often cause strong reactions even in small amounts. - Ice cream and milkshakes
The combination of lactose, sugar, and fat makes these especially problematic for digestion. - Soft, fresh cheeses (ricotta, cottage cheese, cream cheese)
These cheeses retain much of the milk’s lactose and are poorly tolerated by many people with lactose intolerance.

ModerateTolerance varies by portion size and individual
- Yogurt with short fermentation times
Yogurt contains less lactose than milk, but not all yogurts are well fermented. Tolerance depends on bacterial activity and serving size. - Sour cream and crème fraîche
These contain moderate levels of lactose and may be tolerated in small amounts, but not consistently. - Processed foods containing milk powder or whey
Lactose often appears in breads, sauces, dressings, and snacks, sometimes triggering symptoms unexpectedly.
Least Likely: Lower lactose, slower digestion, or minimal lactose
- Long-fermented yogurt (e.g. 24-hour yogurt)
Extended fermentation allows bacteria to break down most of the lactose, making it easier to digest for many people. - Hard, aged cheeses (Parmesan, Grana Padano, Pecorino)
Ageing removes most lactose, leaving mainly protein and fat. - Butter and ghee (clarified butter)
Butter contains only trace amounts of lactose, and ghee contains virtually none, making it well tolerated by most lactose-intolerant individuals.

Kefir and Lactose Intolerance
Kefir is often better tolerated by people with lactose intolerance because it is naturally fermented and contains live bacteria and yeasts that break down much of the lactose during fermentation. In addition, these microorganisms provide β-galactosidase (lactase-like activity), which can help further digest lactose in the gut.
While kefir does not reverse lactose intolerance at a genetic level, regular consumption may improve lactose tolerance and digestive comfort in some individuals by reducing the lactose load and supporting a more adaptable gut microbiome.
As with all fermented foods, tolerance is highly individual, and kefir is suitable only for those with lactose intolerance—not for those with a dairy allergy.
What Is a Dairy Allergy?
A dairy allergy, also known as a milk allergy, is a true food allergy involving the immune system. In this condition, the body mistakenly identifies proteins in milk, most commonly casein or whey, as harmful invaders.
When someone with a dairy allergy consumes milk, the immune system releases chemicals such as histamine. This response can affect multiple organs, including the skin, lungs, digestive tract, and cardiovascular system.
The Food and Drug Administration lists milk as one of the major food allergens because even tiny amounts can trigger serious reactions.
Unlike lactose intolerance, a dairy allergy can lead to anaphylaxis, a life-threatening emergency that requires immediate medical treatment.
Dairy Allergy Symptoms: Why They Can Be Dangerous
Dairy allergy symptoms often appear quickly, sometimes within minutes of exposure. These may include itching, hives, swelling of the lips or throat, vomiting, coughing, wheezing, and difficulty breathing.
The American Academy of Allergy Asthma & Immunology emphasises that breathing difficulty or throat swelling after consuming milk is a medical emergency.
From a clinical nutrition perspective, symptom severity and onset are key indicators that distinguish dairy allergy from lactose intolerance.
Dairy Alternatives for Those with a Dairy Allergy
For individuals with a true dairy allergy, complete avoidance of milk proteins is essential, and lactose-free dairy products are not safe. Fortunately, a well-planned dairy-free diet can still provide key nutrients such as calcium, protein, and vitamin D.
Fortified plant-based milks made from soy, almond, oat, or coconut can help replace calcium and vitamin D, while protein can be obtained from legumes, tofu, tempeh, eggs (if tolerated), nuts, seeds, and fish. One of the simplest and most versatile options is homemade almond milk, which avoids milk proteins entirely and allows full control over ingredients.
Choosing fortified products and including a variety of whole foods is especially important on gluten-free diets, where food choices may already be limited. With careful selection, dairy-free eating can fully support nutritional needs without compromising health.
In Summary – Lactose Intolerance vs Dairy Allergy
One of the simplest ways to understand lactose intolerance vs. dairy allergy is to look at the body systems involved.
Lactose intolerance affects the digestive system, specifically the production of enzymes in the small intestine. Dairy allergy affects the immune system, triggering a systemic defensive response.
This difference explains why lactose intolerance causes gastrointestinal discomfort, while dairy allergy can affect breathing, circulation, and skin.
Health Risks and Long-Term Nutrition Considerations
From a medical standpoint, dairy allergy carries much greater risk. People with this condition must strictly avoid all dairy proteins and often carry emergency medication such as epinephrine.
Lactose intolerance does not pose a medical emergency, but it can impact nutrition if dairy is removed without proper planning. Dairy foods are major sources of calcium, protein, and vitamin D.
As a nutrition student, I often see people unnecessarily cutting out dairy when they could choose lactose-free options to maintain nutritional balance, as I discussed above.
Age, Genetics, and Who Is Most Affected
Lactose intolerance is rare in infants and young children, as infants are born with high levels of the lactase enzyme. It typically develops during adolescence or adulthood as lactase production naturally declines. Genetics play a significant role, and prevalence varies by population.
Dairy allergy is more common in infancy and early childhood. Many children outgrow it, but some carry it into adulthood. The Centers for Disease Control and Prevention identifies milk as one of the most common childhood food allergies.
Understanding when symptoms first appear can help healthcare providers differentiate between the two conditions.
How Lactose Intolerance and Dairy Allergy Are Diagnosed
Lactose intolerance is often diagnosed using hydrogen breath tests, blood glucose tests, or elimination diets. Many people self-identify lactose intolerance, but medical confirmation can help rule out other digestive disorders.
Dairy allergy requires medical testing, such as skin prick tests, allergy antibody blood tests, or supervised oral food challenges. Because reactions can be severe, self-diagnosis is not safe.
Lactose Intolerance and Dairy Allergy at the Same Time?
Yes, although uncommon, some individuals have both lactose intolerance and a dairy allergy. In these cases, lactose-free dairy products are not safe, because they still contain milk proteins.
This distinction is especially important for food bloggers and recipe developers who label dishes as “lactose-free” but not “dairy-free.”
Hidden Dairy: A Major Concern for Allergies
Milk proteins can appear in baked goods, sauces, processed meats, supplements and even medications. While food labelling laws help protect people with allergies, reading ingredient lists remains essential.
For lactose intolerance, trace amounts may be tolerated. For dairy allergy, even small amounts can be dangerous.
When to Seek Medical Advice
Anyone experiencing rapid reactions, swelling, or breathing difficulty after consuming dairy should seek medical attention immediately. Ongoing digestive symptoms should also be discussed with a healthcare provider to ensure nutritional adequacy and rule out other conditions.
FAQs
Is lactose intolerance the same as a dairy allergy?
No. Lactose intolerance affects digestion, while dairy allergy involves the immune system.
Is lactose-free milk safe for those with dairy allergies?
No. It still contains milk proteins.
Can lactose intolerance be dangerous?
No, but it can affect the quality of life and nutrition.
Can children outgrow dairy allergy?
Many do, but not all.
Are plant-based milks healthy alternatives?
Yes, especially when fortified.
Do gluten-free diets increase the risk of nutrient deficiency without dairy?
They can, which is why careful food planning is important.
Fancy a Freebie?
Subscribe for my newsletter
and get your FREE eBook with 7 delicious gluten-free desserts!
*We will only send you gluten-free, lactose-free, refined sugar-free emails; you can unsubscribe anytime. Read our Privacy & Cookie Policy.
In Conclusion:
Understanding the difference between lactose intolerance and a dairy allergy is essential for making safe, informed, and nourishing food choices. One condition requires digestive adjustments; the other requires strict medical caution. From a nutrition student’s perspective, education is the foundation of a healthy gluten-free, lactose-free lifestyle.
Thank you for reading! I hope this article was useful for you.
YourDani x x



About the Author Dani
nutrition student | Healthy Live Promoter | Gluten-free recipe developer
I’m Dani — a final‑year Human Nutrition student with a strong interest in gut health, gluten‑free cooking, UPF-free and whole‑food living.
Your visit really means the world to me.
On DeGlutenista Nutrition, I share simple, science‑informed recipes made without gluten or unnecessary ultra‑processed ingredients. My goal is to show you that living with dietary restrictions can still be delicious, healthy, and deeply satisfying.
My story
My philosophy
References
- National Institute of Diabetes and Digestive and Kidney Diseases – Lactose Intolerance
https://www.niddk.nih.gov - U.S. Food and Drug Administration – Milk Allergies
https://www.fda.gov - American Academy of Allergy, Asthma & Immunology – Milk Allergy
American Academy of Allergy, Asthma & Immunology - Centers for Disease Control and Prevention – Food Allergies
https://www.cdc.gov - Mayo Clinic – Lactose Intolerance vs Milk Allergy
https://www.mayoclinic.org


